
What is a Good Fluid Goal for Polycystic Kidney Disease?
Oct 05, 2022Have you been told to drink more fluid or to stay hydrated? Maybe even read online that it is beneficial for Polycystic Kidney Disease (PKD). That's pretty generic advice…What does it even mean for you?
In this blog, we are going to look into:
- Why hydration is encouraged for PKD
- If is it beneficial to have a higher fluid intake
- Just how much fluid should you should aim for
- All with a side of science to help inspire you to practice your best hydration for PKD
Let's Start With the Science
I am going to start with some science about PKD, the kidneys, and touch on one key hormone you will want to know about! Don’t let this scare you off. Stick with me. Understanding the science will help you move towards putting and keeping, positive hydration habits in place.
Polycystic Kidney Disease
Autosomal Dominant Polycystic Kidney Disease (ADPKD) is caused by the inheritance of the PKD1 gene mutation, which accounts for an estimated 85% of PKD cases, or the PKD2 gene mutations. (1)
The PKD1 and PKD2 genes provide encoding, similar to specific assembly instructions, for making proteins in the body. These proteins, called PC1 and PC2, play a part in:
- Cell growth in the kidneys
- The kidney’s physical structure
- Fluid secretion
PKD gene mutations alter the PC1 and PC2 proteins changing how they interact within the body and the kidneys. This directly affects PKD kidneys:
- Cell growth is connected to cyst growth
- The kidney’s physical structure is altered by cyst fibrosis
- Fluid secretion is elevated, leading to fluid in cysts (2)
Because of the altered genes, some pathways in the body are more active with PKD. I like to think of them as essentially “overstimulated”.
The main “overstimulated” pathway, associated with PKD cyst growth, is called The Vasopressin Pathway. (3) We will come back to vasopressin in a little *hint - this is the hormone you want to know about!
Your Kidneys
I think the kidneys are greatly underappreciated. They play many roles in the body and don't get the credit they deserve. One of their many roles is to maintain fluid balance.
When your body has an excess of fluid, your kidney will increase urine output and get rid of it.
If your body needs more fluid, because every cell and organ in the body needs water to function, your kidneys will reabsorb water and in the process concentrate your urine. This is to prevent dehydration. After all, over 60% of your body is made up of water! (4)
With PKD there is what is called a “urine concentrating defect”. This just means that the kidney’s ability and function to reabsorb fluid is altered. The cause of the urine concentrating defect with PKD is not yet fully understood or known. Because of this defect in concentrating urine, there is a much higher level of the hormone vasopressin with PKD. Which of course is the key hormone in the vasopressin pathway I mentioned earlier!
Vasopressin
Vasopressin is a hormone we all make and use in our bodies. It is frequently called the “anti-diuretic hormone”. Hormones are chemical messengers, vasopressin's primary message is sent to receptors on the kidneys. It is a driver of PKD cyst growth through the stimulation of fluid secretion in the kidneys and cyst cell multiplication.
To understand how good hydration benefits PKD and its progression, let's look at vasopressins’ pathway to the kidneys. (5)
First, vasopressin is released in response to:
- Low body fluid levels *happen well before you “feel” thirsty
- Low blood pressure
- The balance of sodium and electrolytes to fluid in the blood is off balance. This relationship is called osmotic balance.
- Higher blood concentration of particles like sodium and glucose (6)
Second, vasopressin finds its way to receptors on the kidneys, these are called V2 receptors. The V2 receptors are like the gatekeepers to the kidneys.
Third, when vasopressin binds to the V2 receptors it stimulates a chain of events in the kidneys that leads to the kidneys reabsorbing fluid and also fluid secretion within the kidneys. (7) This cascade drives cyst formation and growth. Because of this, vasopressin is a key target for therapy in ADPKD. (8)
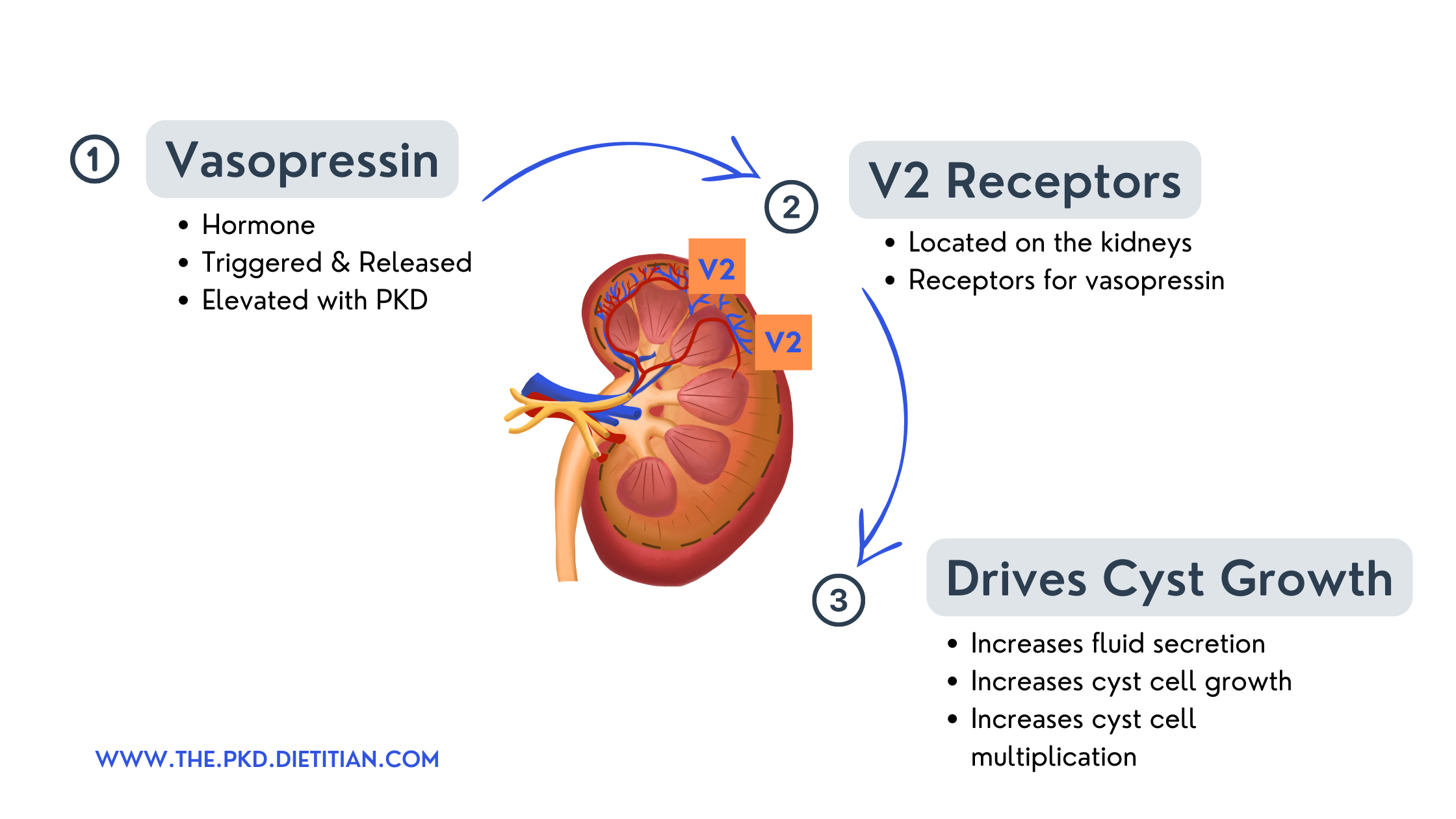
If you are taking Tolvaptan or Jynarque, the V2 receptors might sound familiar. The mechanism, and goal of Tolvaptan & Jynarque, is to block vasopressin from binding to the V2 receptors. That is why they are referred to as "V2 antagonists"!
Diet, Lifestyle, & Vasopressin
With Polycystic Kidney Disease, vasopressin is a main driver of cyst growth. (9) It directly regulates cyst growth. It drives increased fluid secretion to the cyst cells, increases cyst cell growth and multiplication, and higher levels are associated with faster progressing PKD and lower kidney function. (10)
Diet & lifestyle factors that increase vasopressin secretion:
- High sodium intake
- Heavy in protein in
- Smoking
- Poor fluid intake
Both obesity and diabetes are associated with higher circulating levels of vasopressin. (11) All of these are modifiable and can be better managed with diet therapy.
By now you might be thinking of asking your MD if they can check your vasopressin levels…
However, once released in the body, vasopressin has a pretty short lifespan. Because of this, there is no reliable way to directly measure its levels. In clinical studies, copeptin levels are tested and used as a surrogate to assess vasopressin trends (12). This test is not yet commonplace in outpatient care for PKD.
The Rationale Behind “Drink More Fluid”
Increased fluid intake, with your best choice being good old water, helps prevent the additional release of vasopressin. (13) “Enhanced Hydration” is beneficial for combatting PKD, is also good for overall health, is an option available to most people, and has few drawbacks. (14) The whole goal is to interrupt that Vasopressin Pathway!
In animal studies, it has been shown to slow and impair the development and progression of cysts. (15) Human studies are ongoing, and the ones currently published have some flaws in their design. Humans + diet + habits are hard to study for long periods of time!
Benefits of Enhanced Hydration for PKD:
- Reduce stimulation of vasopressin
- Prevent kidney stone and UTI formation, learn more about PKD & Kidney Stones
- Prevents dehydration, which can cause kidney injury and lead to reduced function
How Much Fluid Should You Drink?
The answer is…it depends!
It depends on you. Any dietary recommendation, especially a therapeutic one, should be individualized to you! A good, general recommendation for PKD is to consume 3 liters of water a day.
This is about:
- 100 ounces
- 12 1/2 cups
- 3,000 milliliters

To put that 3 liters/day recommendation in perspective. The adequate recommended fluid intake for general health is 15 cups (3.7 liters) for men and 11.5 cups (2.7 L) for women. (16)
Not too much difference!
I know what you are thinking, what about the recommended 8-8oz cups a day? There is no science behind that at all. It is marketing magic with a catchy, and easy-to-remember phrase.
The goal behind the 3 liters intake recommendation is to generate about 2.5 liters of urine output per day. 2.5+ liters of urine output, in studies like the TEMPO study (17), was the sweet spot for reducing the triggering of vasopressin release. This urine output is also associated with much lower UTI and stone risk. For most people, drinking 3 liters is enough to meet that 2.5 liters of urine output goal.
Some Factors that can increase or decrease your fluid needs are:
- Kidney function < 30 GFR - greater risk of hyponatremia. (18) Talk with MD!
- Exercise
- Meds
- Environment and temperature
- Body size
- If you are pregnant or breastfeeding
How To Tell if You're Hydrated
- Look at the color of your urine
- Is it pale, and almost clear? A sign of good hydration
- Is it darker yellow? This indicates poor hydration and concentrated urine. A sign you need to increase your intake!
- Please note, other things can change the color of your urine like meds, vitamins, and even a burst cyst. Contact your MD if you notice abnormal changes in your urine.
- Look at your labs. Certain markers, like BUN and sodium, are influenced by hydration.
- The best option is to get a 24-hour urine. Your output will be measured and you will know specifically how much urine you are making. Don't change your hydration habits for the test though! A 24-hour urine can also look at sodium output, markers of protein intake, among other components that contribute to urine concentration that are affected by dietary intake.
Can You Drink Too Much Water?
Overhydration and/or holding onto fluid in the body can lead to something called Hyponatremia. This can affect the balance of sodium, fluid, and electrolytes in your body.
The key is to get hydration goals and habits right for you!
It is always best to talk with your doctor or Registered Dietitian and ask how much water is right for you!
Happy Hydration,
Diana, The PKD Dietitian


